Craniopharyngioma are benign (non cancerous) tumours that arise from the sellar region of the brain, near the pituitary stalk
Craniopharyngioma are benign (non cancerous) tumours that arise from the sellar region of the brain, near the pituitary stalk. These often involve the third ventricle, optic nerve, and pituitary gland. Approximately 10-15% of pituitary tumours are craniopharyngiomas. The ones found in children are called Adamantinomatous craniopharyngioma while those occurring in adults (older than 50 years) are called Papillary craniopharyngioma.
Crangiopharyngiomas that represent 2-5% of all primary brain tumours are localised tumours and these often grow in size before being diagnosed. How malignant or how quickly they are likely to spread is totally unknown.
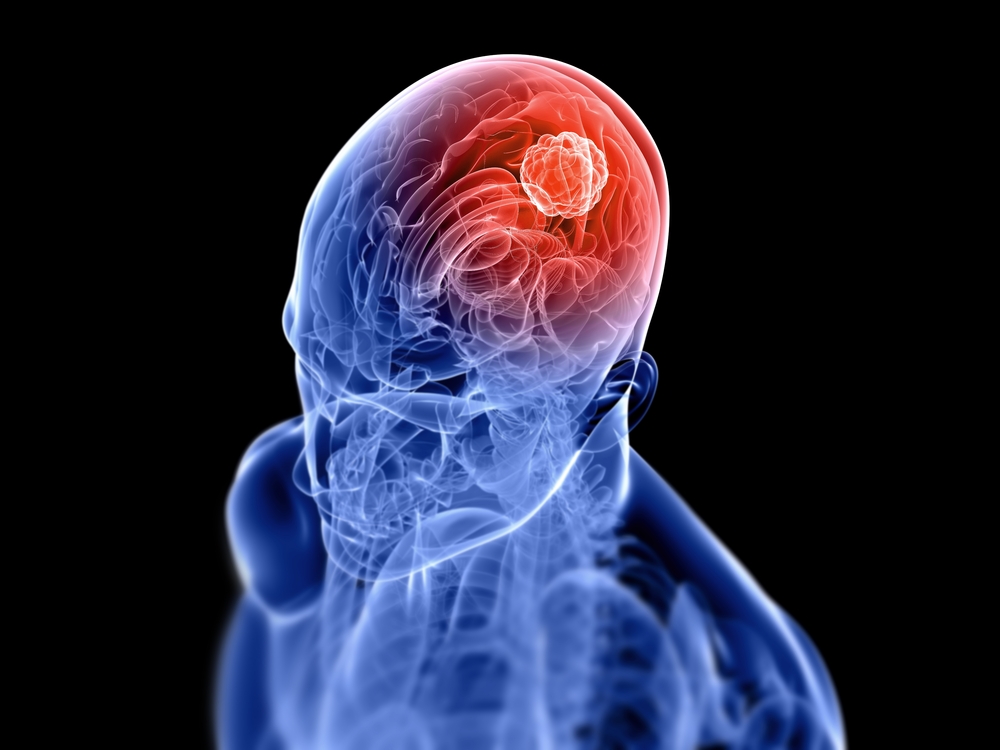
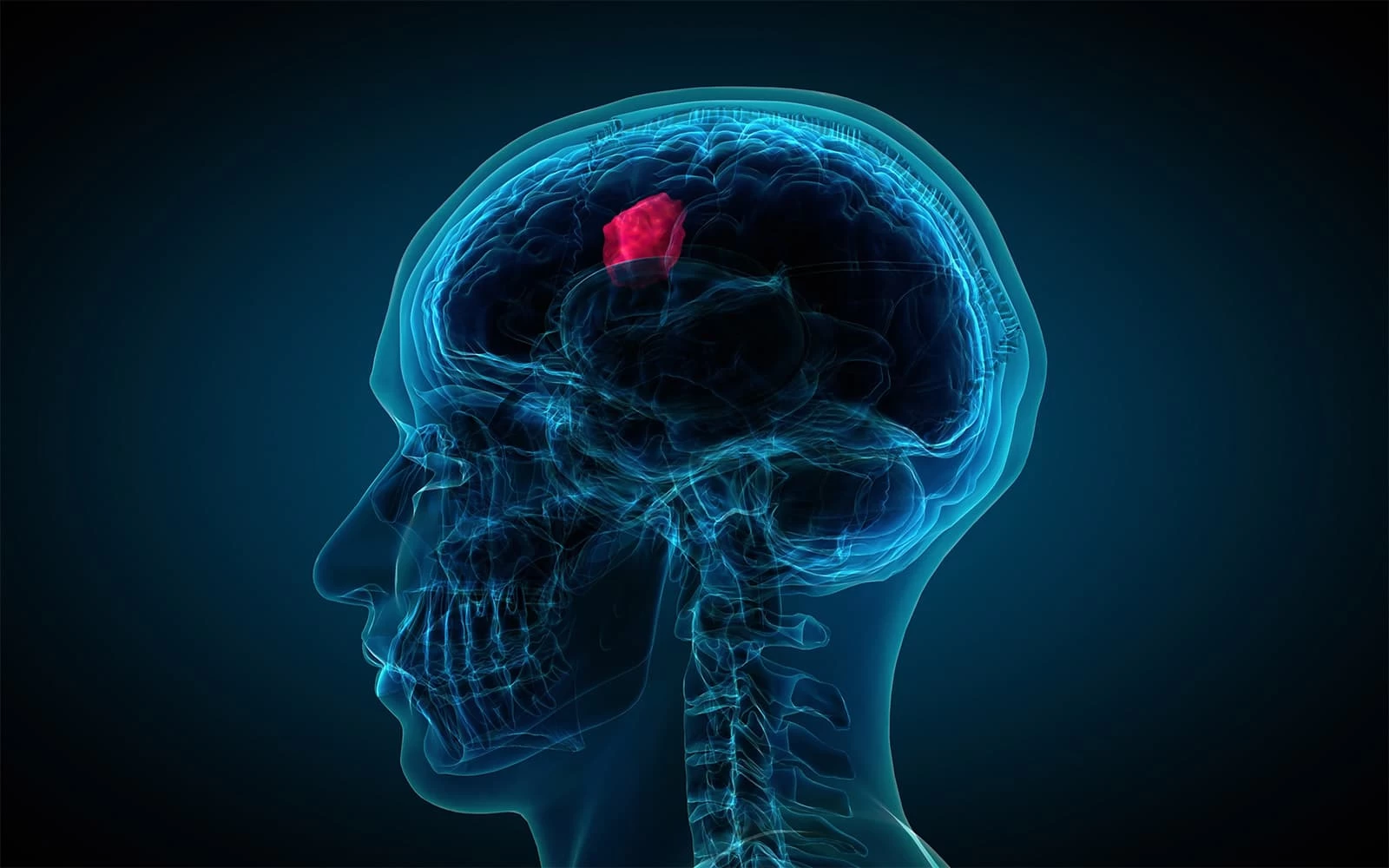
Increased pressure within the brain causes many of the symptoms associated with the tumour. Whereas some symptoms may result from pressure on the optic tract and pituitary gland.
Mood swings, weight change, obesity, delayed development, impaired vision, and a swollen optic nerve are common among patients of craniopharyngioma.
Blood and urine tests to measure hormone levels and medical imaging provide the best means of diagnosing pituitary tumours. For craniopharyngiomas, an MRI of the area surrounding the pituitary gland is performed. In addition, a CT scan may be performed to provide a detailed image of the brain and pituitary gland.
Specific treatment for a craniopharyngioma is determined by the neurosurgeon and endocrinologist. Based on the specific nature of the patient’s craniopharyngioma, treatment may include surgical removal of the tumour, including a procedure called craniotomy, radiosurgery or stereotactic radiotherapy, or hormonal replacement therapy.
However, surgery to remove the tumour is usually the first step in treatment. If hydrocephalus (excess water in the brain) is present, a shunt (drainage system) may be placed during surgery. This helps to remove excess cerebrospinal fluid from the brain and ease the pressure.
Radiation therapy may be suggested if entire tumour cannot be removed. In children younger than 3 years, radiation may be delayed by the use of surgery or hormone therapies.
Copyright © 2020. All Rights Reserved.
Designed and Developed by Easy Solution 360